By Neil White, Professor of Intelligent Sensor Systems at University of Southampton
What we're trying to solve
As someone who's spent the past decade working at the interface between sensor technologies and healthcare, I'm always struck by how the simplest physiological parameters are the most challenging to measure well. Respiratory rate is a perfect example. It's one of the earliest indicators that a patient’s condition may be deteriorating, yet also one of the least reliably recorded, owing largely to the fact that it's still commonly measured by manually counting breaths.
Despite its clinical importance, respiratory rate remains the most inconsistently measured vital sign. Manual counting is prone to error, intermittent and time consuming. Clinicians are aware of these limitations, yet alternative automated systems (chest straps, face mounted sensors, airflow monitors) can be uncomfortable, obtrusive and ill-suited to prolonged use.
The need for better solutions is urgent. Globally, more than 435 million people live with chronic respiratory diseases including asthma and COPD. For these individuals, the ability to track breathing continuously and non invasively could transform both diagnosis and ongoing management.
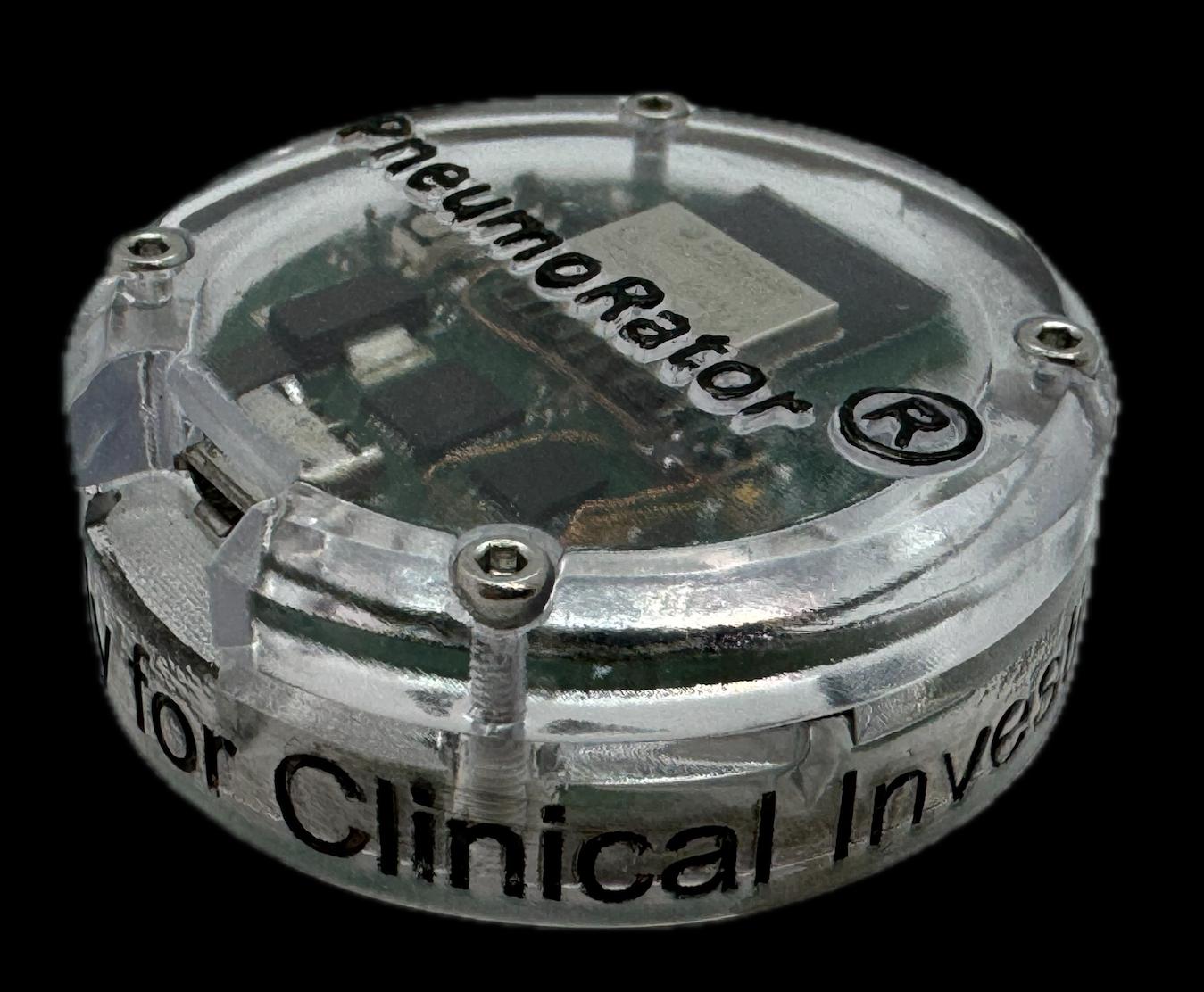
Our aim with the PneumoRator® has been to develop a clinically robust sensor that people would actually want to wear - one that is comfortable, accurate and seamlessly integrated into routine care.
How the PneumoRator® Works
 The PneumoRator® is constructed from a novel form of capacitance-based sensor. Rather than relying on tight chest bands or direct skin contact, the device detects subtle variations in capacitance caused by natural chest wall movement and the stretching of the skin during breathing. What makes this approach particularly powerful is its non-intrusive nature. The sensor can operate through clothing, avoiding the discomfort and inconvenience associated with many existing wearable respiratory monitors.
The PneumoRator® is constructed from a novel form of capacitance-based sensor. Rather than relying on tight chest bands or direct skin contact, the device detects subtle variations in capacitance caused by natural chest wall movement and the stretching of the skin during breathing. What makes this approach particularly powerful is its non-intrusive nature. The sensor can operate through clothing, avoiding the discomfort and inconvenience associated with many existing wearable respiratory monitors.
During controlled testing with healthy volunteers performing everyday movements, the PneumoRator® demonstrated continuous monitoring with an accuracy of around ±2 breaths per minute. Further clinical validation at University Hospital Southampton (UHS), including patients undergoing a range of surgical procedures, showed the device performs comparably to gold standard capnography, the current clinical benchmark.
Designed for Real World Clinical Use
Beyond accuracy, a major advantage of the PneumoRator® is its suitability for large scale manufacture. The materials and fabrication processes have been carefully chosen to ensure the device remains low-cost, making widespread deployment in hospitals and community care entirely feasible.
 Once implemented in practice, we envisage the PneumoRator® communicating wirelessly with a dedicated smartphone or tablet application. Healthcare teams will be able to view patients’ respiratory data in real time and receive automated alerts when significant changes occur - supporting faster, more informed clinical decision making.
Once implemented in practice, we envisage the PneumoRator® communicating wirelessly with a dedicated smartphone or tablet application. Healthcare teams will be able to view patients’ respiratory data in real time and receive automated alerts when significant changes occur - supporting faster, more informed clinical decision making.
A Collaborative Journey
The PneumoRator® project has been made possible through the expertise and dedication of a multidisciplinary team. The work is a collaboration between the University of Southampton, University Hospital Southampton, and Nottingham Trent University, supported by medical technology company Zelemiq Ltd.
We have been fortunate to receive nearly £1 million in funding from the National Institute for Health Research (NIHR), and the ongoing development is being advanced within the NIHR Southampton Biomedical Research Centre.
Looking Ahead
We believe the PneumoRator® represents an important step toward improving how respiratory rate is monitored in clinical and community settings. By providing continuous, comfortable, and reliable respiratory data, the system has the potential to help clinicians identify early signs of deterioration, streamline patient monitoring, and improve outcomes for millions of people worldwide.
As we continue refining the technology and preparing for wider deployment, our goal remains clear: to turn respiratory monitoring from one of the most overlooked aspects of patient assessment into one of the most reliable.
If you'd like to find out more please email me nmw@ecs.soton.ac.uk

 The PneumoRator® is constructed from a novel form of capacitance-based sensor. Rather than relying on tight chest bands or direct skin contact, the device detects subtle variations in capacitance caused by natural chest wall movement and the stretching of the skin during breathing. What makes this approach particularly powerful is its non-intrusive nature. The sensor can operate through clothing, avoiding the discomfort and inconvenience associated with many existing wearable respiratory monitors.
The PneumoRator® is constructed from a novel form of capacitance-based sensor. Rather than relying on tight chest bands or direct skin contact, the device detects subtle variations in capacitance caused by natural chest wall movement and the stretching of the skin during breathing. What makes this approach particularly powerful is its non-intrusive nature. The sensor can operate through clothing, avoiding the discomfort and inconvenience associated with many existing wearable respiratory monitors. Once implemented in practice, we envisage the PneumoRator® communicating wirelessly with a dedicated smartphone or tablet application. Healthcare teams will be able to view patients’ respiratory data in real time and receive automated alerts when significant changes occur - supporting faster, more informed clinical decision making.
Once implemented in practice, we envisage the PneumoRator® communicating wirelessly with a dedicated smartphone or tablet application. Healthcare teams will be able to view patients’ respiratory data in real time and receive automated alerts when significant changes occur - supporting faster, more informed clinical decision making.